Vitamin D supplementation has a protective effect, against the incidence of COVID-19 in RCT studies.
Bacteria

It is said that about half of the entire human population plays host to H. pylori, but not much is known about how this bacterium manages to colonize and persist inside the human stomach. In a new study published in the journal PLOS Biology, researchers from the U.S. and the U.K. addressed this by investigating the behavior of H. pylori in the stomach of mice. Using high-resolution imaging and mapping techniques, they were able to observe and present a new model of how the bacterium establishes colonies, survives, and thrives in the stomach of living organisms.
Helicobacter pylori: symptoms and complications
H. pylori infections often occur during childhood. The bacterium then remains in the stomach of an infected individual throughout much of his or her life. But unlike other pathogenic bacteria, H. pylori doesn’t cause sickness. In fact, some people naturally have such a high resistance to the bacterium that infection causes them no harm. On the other hand, people who are less fortunate can suffer from ulcers or cancer caused by H. pylori infection.
Because H. pylori infection almost never shows any signs or symptoms, most people don’t realize they are infected until they experience the complications. On the rare occasion that symptoms manifest, they normally include:
- Abdominal pain or a burning sensation
- Bloating
- Frequent burping
- Loss of appetite
- Nausea
- Weight loss
Meanwhile, complications that may arise due to H. pylori infection include:
- Peptic ulcers
- Inflammation of the stomach lining
- Gastric cancer
According to a study, about 75 percent of the global gastric cancer burden and 5.5 percent of malignancies worldwide can be attributed to inflammation and injury caused by H. pylori. Unfortunately, the mechanisms involved in H-pylori-related cancer development are still unknown. (Related: The symptoms and dangers of an H. pylori infection.)
The nature and behavior of H. pylori inside the stomach
Despite the stomach’s high acidity, H. pylori can still survive and even thrive in it for years. People with H. pylori infection are given antibiotics to control the infection, but even these modern drugs cannot completely eliminate the bacterium. After a while, the same bacterial colonies regrow in the stomach. This phenomenon has led scientists to believe that H. pylori has a hiding place somewhere in the stomach where it can safely regenerate after antibiotic treatment.
To further explore this possibility, the researchers used a mouse model that they infected with two strains of the bacterium: one with a green fluorescent marker and one with a red fluorescent marker. Using 3D microscopy and a passive CLARITY technique (PACT) that makes tissue optically transparent, they analyzed the intact stomachs of infected mice and observed where H. pylori chose to settle in that organ.
The researchers reported that H. pylori establishes itself in the stomach by colonizing a specialized microenvironment or microniche deep in the gastric glands. These glands are small branched tubules found in the stomach lining and possess only one entrance, the size of which is just enough to accommodate the bacterium. Once H. pylori has successfully established colonies, it then expands to adjacent glands and starts forming clonal population islands that persist over time.
The researchers observed other interesting things about the bacterium’s behavior. For one, H. pylori populations that form in gastric glands do not mix with free-swimming bacteria in the surface mucus. In fact, gland-associated H. pylori compete for space and prevent other bacteria from establishing colonies in the stomach. The researchers also found that the host’s age upon infection and immune responses influence the bacterial density inside the gastric glands.
Based on their findings, the researchers concluded that H. pylori creates a reservoir inside the stomach by colonizing gastric glands, and this reservoir is what replenishes the population of H. pylori in the stomach after antibiotic treatment and allows H. pylori infection to persist for a very long time.
Sources include:
realfarmacy.com
Source: Spirit Science
June 10, 2019
The practice of smudging dates back to prehistoric times, and is still very much in use today worldwide for cleansing everything from dwellings to human spirits. However recent research has shed light on the popularity of this activity, revealing that burning certain plant matter actually clears harmful bacteria.
All Western use of burning herbs and plants for spiritual purposes aside, the activity rests firmly in the sensibilities of ancient cultures in that, historically, smudging was believed to put forth the spirits of various ‘allies’ to provide ease and balance to an individual or group.
In this way, the practice was used to clear spiritual and emotional negativity that has built up in a body or a space.
Of course, there are skeptics who belittle the practice as unscientific and akin to magic.

The practice has a negative association to a form of cultural imperialism, where traditions of dwindling indigenous populations are co-opted by the descendants of those who more-or-less conquered them.
The scientific paper entitled “Medicinal Smokes” and published in the Journal of Ethnopharmacology focuses a scientific lens on the practice, which is becoming more and more widely practiced, despite skepticism.
It serves to play against the role that this activity has played in a culturally diverse range of religions and tribal beliefs.
The research study looked into herbal and non-herbal remedies that were administered by the burning of various matter.
The research included information from 50 countries over 5 continents and found that, predominantly, smoke administered medicinally is mostly used to aid lung, brain and skin function. In addition, it was revealed that passive fumes doubled as a sort of air purifier.
The purpose of the study was to see whether or not these medicinal smoke deliveries could be explored by western medicine, because “The advantages of smoke-based remedies are rapid delivery to the brain, more efficient absorption by the body and lower costs of production.”
A follow up paper published in the same periodical, “Medicinal smoke reduces airborne bacteria,” found that the research concluded that, in addition to health benefits, smudging was a powerful antiseptic.

“We have observed that 1 hour treatment of medicinal smoke emanated by burning wood and a mixture of odoriferous and medicinal herbs (havan sámagri=material used in oblation to fire all over India), on aerial bacterial population caused over 94% reduction of bacterial counts by 60 min and the ability of the smoke to purify or disinfect the air and to make the environment cleaner was maintained up to 24 hour in the closed room.
Absence of pathogenic bacteria Corynebacterium urealyticum, Curtobacterium flaccumfaciens, Enterobacter aerogenes (Klebsiella mobilis), Kocuria rosea, Pseudomonas syringae pv. persicae, Staphylococcus lentus, and Xanthomonas campestris pv. tardicrescens in the open room even after 30 days is indicative of the bactericidal potential of the medicinal smoke treatment.
We have demonstrated that using medicinal smoke it is possible to completely eliminate diverse plant and human pathogenic bacteria of the air within confined space.”
In short, burning medicinal herbs cleared airborne bacterial populations by 94%, and the space was still found to be disinfected a day later. What’s more, a month after smudging, much of the pathogens originally found were still undetectable.
This has profound implications, as modern air quality in the developed and undeveloped world is atrocious, containing up to 1,800 bacterial types, many of them pathogenic. With an increasing deadly array of antibacterial-resistant strains, we’ll need all the help we can get.
Conventional methods of sterilization often employ chemical cocktails that are typically much less effective than purported. Smudging seems to be an effective alternative, while also being natural and safe to use.
In conclusion, the ancient practice of burning powerful herbal material may be much much more than just a primitive belief that we can simply disregard due to it being unscientific.
Of course, this should not take away from the properties of smudging in the area of energy system and soul cleansing and in the power of aromatherapy.
Candida auris is a “silent superbug” that’s already spreading across U.S. hospitals and nursing homes. The CDC has reported hundreds of infections
Source: Candida Auris: The Silent Superbug That’s Already Too Late to Stop
realfarmacy.com
May 5, 2019
Candida auris is a “silent superbug” that’s already spreading across U.S. hospitals and nursing homes. The CDC has reported hundreds of infections across seven states, and is tracking over 1,000 “colonizations” where the fungal strain has infected human carriers who spread it to others.
Notably, the CDC refuses to name which hospitals have been infected by Candida auris, even as it admits infections are spreading across Illinois, New Jersey and New York.
It has also spread across the world, with hospital-related infections documented in several countries. The following map is published by the CDC:

According to the CDC, people infected with Candida auris have a 50% chance of being killed by it within 90 days.
There is no vaccine, which is probably why the corporate media almost never mentions this superbug. Even worse, this superbug fungal strain is a product of chemical agriculture, and as long as the agricultural giants continue to inundate crops with fungicides, more fungal superbugs are going to emerge and threaten humanity.
We’ve produced and posted a full 46-minute Counterthink episode that documents this emerging threat to humanity. Watch it exclusively at Brighteon.com, the YouTube alternative for free speech videos on science, medicine, health and more.
Source: Naturalnews.com
“The harsh fact is nearly one-half of patients that contract C. auris die within 90 days.”
With permission from
APRIL 12, 2019
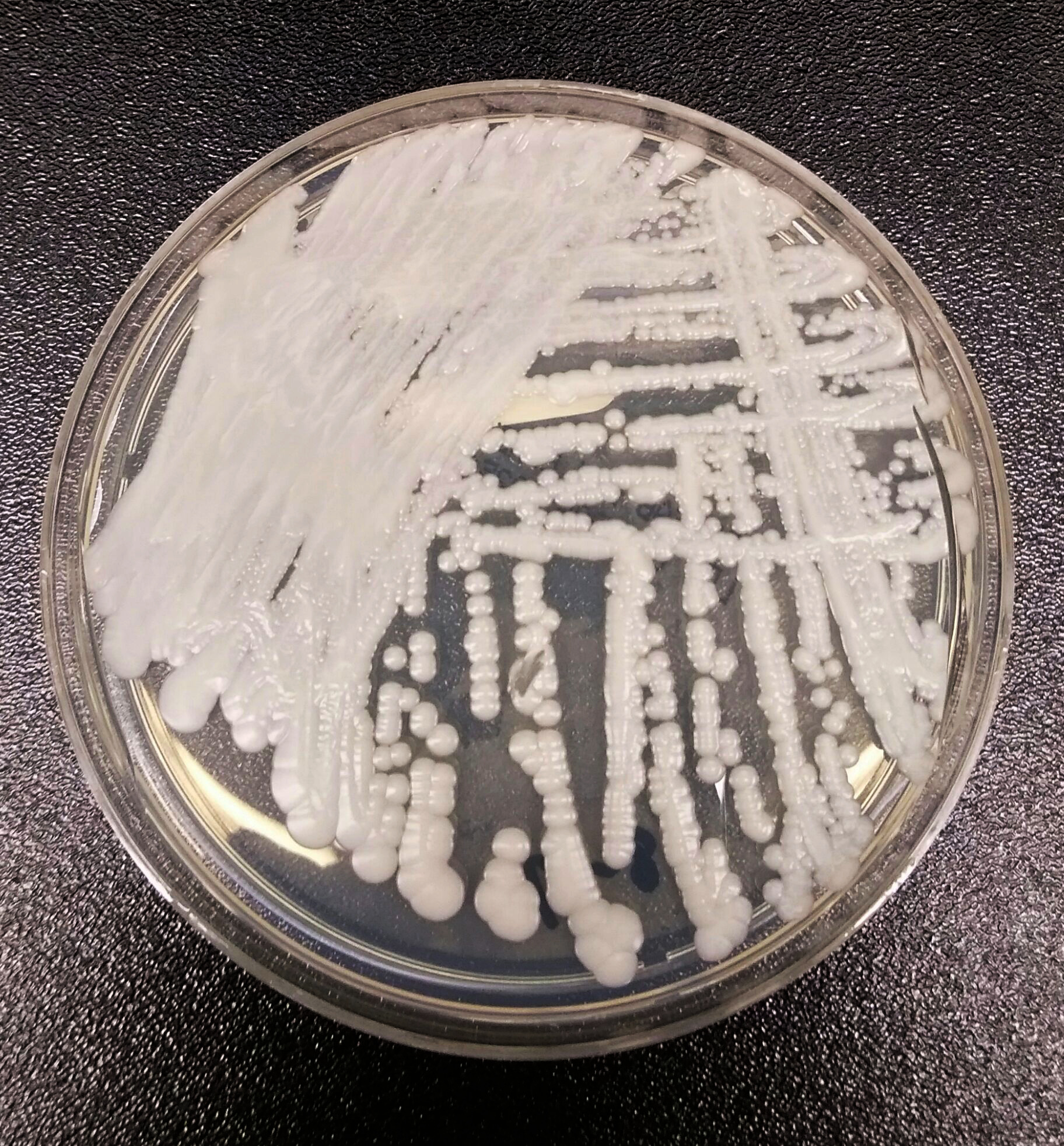
Candida auris
Public health experts have been warning for decades that overuse of antibiotics reduces the effectiveness of drugs that cure bacterial infections. At least 2,000,000 Americans get antibiotic-resistant infections per year.
Notably, gluttonous overuse of antimicrobial drugs to combat bacteria and fungi via hospitals, clinics, and farms is backfiring and producing superbugs or “Nightmare Bacteria,” which is especially lethal for people with compromised immune systems and autoimmune disorders that use steroids to suppress bodily defenses.
Federal Centers for Disease Control and Prevention (“CDC”) recently labeled a fungus called Candida auris or C. auris an “Urgent Threat.” This Nightmare Bacteria is a brutal killer that’s unstoppable and flat-out travels fast.
The CDC claims antibiotic resistance is “one of the biggest public health challenges of our time.”
According to the World Health Organization: “The world is facing an antibiotic apocalypse.”
The UK’s chief medical officer believes antimicrobial resistance: “May spell the end of modern medicine,” as routine surgeries turn into medical emergencies.
In short, new antibiotic resistance mechanisms are emerging and spreading worldwide, quickly. Knowledgeable sources worry that society at large is headed for a “Post-Antibiotic Era,” in which common infections and minor injuries can kill once again (Source: WHO Fact Sheet on Antibiotic Resistance, Nov. 2017).
According to a recent British governmental study, without new medicines and without curbing unnecessary use of antimicrobial drugs, infections followed by ensuing deaths will likely eclipse cancer deaths over succeeding decades. The harsh fact is nearly one-half of patients that contract C. auris die within 90 days. (Source: Pew Campaign on Human Health and Industrial Farming)
Nowadays, the dangers of “Nightmare Bacteria” are growing out of control. The latest concern is that C. auris will begin spreading to healthier populations, even though healthy people are normally not at risk. Within only five years, C.auris has established itself as one of the world’s most intractable health threats. It is drug-resistant, tenacious and nearly impossible to exterminate and travels the globe looking for innocent victims, killing people mostly in hospital settings.
C.auris has already established a beachhead in Venezuela, Spain, the UK, India, Pakistan, South Africa, New York, New Jersey, and Illinois. Nobody knows where else it may be cloaking.
A British hospital aerosolized hydrogen peroxide in a C.auris-infected room for one week solid. Subsequently, only one organism grew back in a Petri dish in the room. It was C. auris. The hospital serves wealthy patients from Europe and the Middle East, and it has not made a public announcement of the outbreak.
An outbreak of C.auris at a Spanish hospital resulted in 41% deaths of infected patients. The hospital has not made a public announcement of the outbreak.
In the U.S., the Brooklyn branch of Mount Sinai Hospital had a case of C. auris with an older man hospitalized for abdominal surgery.
According to a New York Times article d/d April 7th 2019: Deadly Germs, Lost Cures: A Mysterious Infection, Spanning the Globe in a Climate of Secrecy: “The man at Mount Sinai died after 90 days in the hospital, but C. auris did not. Tests showed it was everywhere in his room, so invasive that the hospital needed special cleaning equipment and had to rip out some of the ceiling and floor tiles to eradicate it… C. auris is so tenacious, in part, because it is impervious to major antifungal medications, making it a new example of one of the world’s most intractable health threats: the rise of drug-resistant infections.”
Indeed, Mount Sinai’s public exposure is an exception, as hospitals and governmental agencies keep C.auris’s whereabouts secret. Public transparency is shunned. Hospitals and local governments are reluctant to disclose outbreaks because of concern about tarnishing reputations and spreading of rumors. Even the Center for Disease Control is not allowed, in a pact with states, to publicly announce outbreaks.
There are multiple causes behind antibiotic-resistant infection outbreaks. As for one, using antifungals on crops to prevent rotting, in turn, contributes to drug-resistant fungi infecting people. Also, infamously, antibiotics are widely used (in fact, overused-by-a-country-mile) for disease prevention of farm animals.
“Indeed, researchers estimate that up to 70 percent of all antibiotics sold in the U.S. are given to healthy food animals to artificially expedite their growth and compensate for the effects of unsanitary farm conditions. This routine use of antibiotics in animals presents a serious and growing threat to human health because it creates new strains of dangerous antibiotic-resistant bacteria.” (Source: How Much Do Antibiotics Used on the Farm Contribute to the Spread of Resistant Bacteria? Scientific American magazine)
Furthermore, and of serious deliberate interest, Denmark is testament to what occurs by restricting non-therapeutic use of antibiotics in cattle, broiler chickens, and swine. Following Denmark’s restrictions, the use of antibiotics for swine dropped 50% from 1992-2008. Results: (1) swine production increased by nearly 50% and (2) antibiotic resistance in humans decreased.
By way of contrast, in the United States up to 70% of antibiotics go to farm animals that are not sick.
One pressing issue is no new classes of antibiotics have been invented for decades. In fact, all the antibiotics brought to the market in the past 30 years have been variations on existing drugs discovered by 1984, meaning they are just follow-up compounds, without a novel mechanism of action, meaning no major breakthroughs.
Problematically, only a few large drug companies are involved in antibiotic research and development because the cost of developing the drugs is high and profit margins are slim. In that regard, according to the Center for Infectious Disease Research and Policy: The antibiotic pipeline is near collapse, and the country needs to act now to preserve the infrastructure to support antibiotic research and development.
Pew Charitable Trust/Antibiotic Resistance Project is trying to muster public support for the Preservation of Antibiotics for Medical Treatment Act (PAMTA, H.R. 1587/S. 619), which withdraws from animal production use of seven classes of antibiotics vitally important to human health, unless animals are diseased or drug companies can prove that their use does not harm human health.
Other groups in support of legislation include the American Medical Association, American Academy of Pediatricians, Infectious Diseases Society of America and World Health Organization.
In a letter to congressional leaders Feb. 5, 2019 The Pew Charitable Trusts, Infectious Diseases Society of America, and Trust for America’s Health, together with U.S. antibiotic developers large and small, called on Congress to move swiftly to enact a package of economic incentives to reinvigorate the stagnant pipeline of antibiotics.
A number of sponsors for congressional action are urging concerned citizens to call their representatives and senators and push for action on this life-or-death issue.
Kombucha’s unlikely rise from Soviet elixir to modern-day miracle drink.

May 2018
In May of 1995, Ruth Patras realized that something was wrong with her 5-week-old daughter, Ciara. Initially happy and healthy, about a month after Ciara was born, the whites of her eyes started to turn yellow. Over the next few days, the color deepened, and her appetite diminished. Patras took Ciara to her pediatrician, who sent the family to Children’s Hospital of Philadelphia. Tests revealed that Ciara had biliary atresias, a rare liver disease in which the ducts that pass bile from the liver to the gallbladder and the first section of the small intestine become blocked. Bile serves two functions in the body, helping to digest fat and carry waste out of the liver. When trapped, the excess bile damages liver cells, eventually leading to liver failure.
Doctors told Patras that the only hope for Ciara was a complex surgery known as the Kasai procedure, in which the gallbladder and bile ducts are removed and the liver is connected directly to the small intestine. The Kasai procedure is hardly a cure, though: It’s only successful 30 to 50 percent of the time, and when it fails, patients need a liver transplant as early as age 1 or 2; even when it works, around three-quarters of patients still require a liver transplant by their 20th birthday.
After the procedure, doctors explained, the rest was up to Ciara’s immune system. Hearing this, Patras felt the first spark of hope she’d had since the diagnosis. She walked out of the room, away from other shell-shocked parents, to the pay phone at the end of the hall, where she called her husband. She told him that she was bringing the baby home that weekend, and that he needed to open a package that was waiting on the kitchen counter.
While pregnant with Ciara, Patras had heard a guest on the daytime talk show Leeza discussing a drink that could boost the immune system. Patras had already lost her mother, uncle, several aunts, and both grandmothers to cancer, so strengthening her immune system seemed appealing. She ordered a kit to make the beverage, a fermented tea called kombucha.
Through the confusing whirlwind of doctor’s appointments leading up to Ciara’s diagnosis, Patras began bottle-feeding kombucha to her sick child. One week after Ciara underwent the Kasai procedure, Patras continued the kombucha regimen. Ciara’s pediatrician objected, but within a few weeks, bile began to drain from her liver, and in follow-up exams, Ciara’s liver appeared softer and smaller. Patras knew this could be the result of a successful Kasai procedure, but suspected that, somehow, the kombucha was involved. She waited nearly a year before telling Ciara’s pediatrician about it again. When she did, the doctor ordered her to stop giving it to Ciara immediately. “She actually reprimanded me,” Patras told me.
The doctor said that there was no scientific evidence for kombucha’s safety or efficacy, but Patras didn’t need any: Her daughter’s health was proof enough.
Some $600 million worth of kombucha was sold last year, peddled everywhere from bodegas to bars to Bed Bath & Beyond. It’s on tap at cool coffee shops; it’s in your neighbor’s fridge; it’s on Entourage and The Mindy Project and Flaked. Its ubiquity in post-Portlandia America has been largely powered by the reverberations of the claims that attracted Patras over 20 years ago: that it supports digestion, metabolism, cell integrity, immunity, appetite control, weight control, liver function, and healthy skin and hair — or as artsy labels put it today, by promises that it will “rejuvenate, restore, revitalize, recharge, rebuild, regenerate, replenish, regain, rebalance, renew.”
A small fraction of today’s kombucha drinkers consume it in hopes of curing cancer or alleviating psoriasis. The vast majority are just taking part in the recent aspirational hegemony of “wellness” — the cultural tidal wave that has given us skincare as coping mechanism, turmeric lattes with almond milk, and brain dust — hoping that kombucha might be part of the recipe, whether it balances their microbiome or simply boosts their energy levels.
Bruce Chassy, a professor emeritus in the department of food science and human nutrition at the University of Illinois at Urbana-Champaign, says there’s a short explanation for why people have turned to kombucha to be healthy, or at least for a whiff of wellness: “More and more people are mistrusting of many, many different things, whether it’s politicians or corporations or traditional medicine.”
Americans are choosing to believe in their intuition, to choose whole foods and natural products instead of processed foods and pills. “The more important part of this is that people have changed remarkably in what they will consider as evidence or reason for forming an idea about something,” Chassy says. “We’re inundated with information and conflicting claims. People are believing what they want to believe, and ignoring the rest.” (Case in point: The debate over genetically modified organisms, in which Chassy is embroiled after documents showed that he accepted money from Monsanto even while presenting himself as an independent academic researcher.) Seeded by dubious prophets with tidings of good health, and stoked by thrifty entrepreneurs, the kombucha phenomenon took root in America at a perfect moment — just as some people began to lose trust in modern medicine and wanted to believe in something more.
A few months before Ruth Patras heard kombucha touted on a daytime talk show, a group of housemates in Portland, Oregon, tried it for the first time after a friend left some behind. One of them, Robert Deering, was especially intrigued. Deering holds a BS in biology from the University of California, Santa Cruz and a master’s in microbiology from the University of Washington; after grad school, he spent a few years working in a cancer research lab in Seattle before moving to Portland. Curiosity led him to the library at nearby Portland State, where he found a 1940s book on fermentation with a short section on kombucha. It explained that kombucha starts with a SCOBY — a symbiotic culture of bacteria and yeast — which forms in the organic compound cellulose.

In your hand, a SCOBY feels like Play-Doh that’s soaked in water; in the bottom of your glass, it looks about as appetizing as a loogie. Kombucha is produced when a SCOBY is combined with sugar and brewed tea — black, oolong, or green, as long it’s from the tea plant, Camellia sinensis. The entire process takes about two weeks. First, the sugar and hot tea are combined. Once the sweetened tea has cooled, an acidifier — often matured kombucha — can be added to prevent unfriendly bacteria. Then the SCOBY is placed on top and the container is covered with a breathable cloth, so that air can get in but dust and fruit flies can’t. As the SCOBY lowers the pH of the sweetened tea, its rising acidity kills off pathogenic bacteria, and acid-tolerant microbes consume the oxygen in it, beginning fermentation. When the oxygen is gone, the yeast starts breaking down the sugar, converting it to alcohol; the bacteria in the SCOBY then breaks that down to form various acids, resulting in the final product: kombucha. It smells like diluted vinegar and malty yeast, and when poured into a glass, it bubbles like champagne. Once bottled, the bubbles remain, making it more interesting than water, less sweet than juice, and less potent than soda.
Deering learned that no two SCOBYs are exactly the same, and no two batches of kombucha are exactly alike, in part because each batch picks up different yeast microbes from the air. Room temperature and the water also affect the flavor, the speed of fermentation, and the development of gases. Alcohol continues forming as long as there is yeast and sugar in the mixture, so the final alcohol content depends on when the SCOBY is removed, or when the kombucha is pasteurized. If kept unpasteurized, or raw, fermentation continues, and so does alcohol production. When treated properly, each SCOBY can be used to start a new batch — or two, because every few days SCOBYs sprout a thin layer of cellulose that easily peels off the bottom and can be used on its own.
Science has yet to offer a better explanation of how kombucha develops than what Deering found in that 70-year-old book, and no one has definitively determined where the first SCOBY came from — only that kombucha has almost always been synonymous with miraculous health claims.
Egyptologist Zahi Hawass once claimed kombucha was first brewed during the reign of Khufu, who commissioned the Great Pyramid, around 2500 BCE; The Big Book of Kombucha points to a legend claiming it originated in northern China in the third century BCE, but wasn’t regularly consumed there until the seventh century CE at the earliest; authors Harald Tietze, Andra Anastazia Malczewski, and Marie Nadine Antol each claim a Korean physician named Kom-bu brought it to Japan in 414 CE, as he attempted to treat the Emperor Inkyo’s various disorders. Some say Genghis Khan’s armies carried it west, others say it traveled along the Silk Road. Whatever its ancient origins, German scientists were referencing it in their work by the 1850s.
Dozens of far-fetched stories detail the drink’s healing powers. In one tale, people live to over 100 in the 8,500-person village of Kargasok on the Ob River because they drink kombucha. There, legend has it that kombucha allowed an 80-year-old woman to give birth to her first child, fathered by a 130-year-old man. Russian and German doctors mentioned kombucha in more than 100 publications between 1917 and 1935. During that time, it came to be known as the “tea of immortality” in various parts of Europe; in France, it was known as l’élixir de longue vie.
These claims traveled predominantly by word-of-mouth, including informational leaflets, until 1994, when Tietze, a German-born kombucha drinker, perpetuated its mythos in a dubiously sourced book called Kombucha: The Miracle Fungus, which claimed to summarize the various medical benefits that European doctors, as well as people who wrote him letters, ascribed to kombucha — and which devoted kombucha drinkers once pointed to as evidence of its medical efficacy. Tietze describes, for instance, a 1987 study by Reinhold Weisner, a possibly made-up physician and biologist working in Bremen, Germany, who conducted a trial with 246 patients to compare kombucha treatment with Interferon, a common immune-boosting drug used in the treatment of various illnesses. According to Tietze, Weisner found kombucha more effective in treating asthma, 92 percent as effective in treating rheumatism, and 89 percent as effective on kidney disorders. (“There’s a long history of bad studies coming out of the former Soviet Union,” Chassy notes. “The medicine was deeply rooted in folk beliefs, and what they wanted to come out influenced what came out.”)
Tietze questionably claims that kombucha made its first voyage across the Atlantic Ocean on the strength of those Soviet health studies, when Ronald Reagan was diagnosed with cancer in 1985. According to Tietze’s fantastical account, Reagan read the semi-autobiographical novel of Nobel Prize recipient Aleksandr Solzhenitsyn and credited kombucha with helping him overcome cancer in the 1950s; inspired, Reagan acquired a SCOBY from Japan and started drinking a liter of kombucha every day, stopping the cancer from spreading. (Reagan in fact had a polyp and two feet of his lower intestine surgically removed.)

The White House has never confirmed whether Reagan drank kombucha, and it’s not mentioned in any official biographies — if he did drink it, he was one of the few known to do so outside niche hippie communities in the U.S. until 1992, when it emerged on the alternative health scene in California. (A mycologist in Olympia, Washington, once told the New York Times that a pharmaceutical company asked him to research kombucha in 1980.) That year, a German-born instructor offered it to a class at an LA meditation center, saying it would “help heal the planet.” In that meditation group was a graphic designer named Betsy Pryor, who might have been the first person to commercialize kombucha in the U.S. “One evening after class, where I’d silently asked God to help me keep people alive … the meditation instructor emerged from the center kitchen clutching an odd, pancake-looking thing encased in a clear plastic bag,” Pryor wrote on her now-defunct website. “[The instructor] paused, looking at me intently. ‘It’s going to help heal the planet.’ A few weeks after I started to drink the Kombucha Tea, I felt like I’d been reborn.” An immediate believer, Pryor and her partner began selling SCOBYs by mail order the next year, charging $50, or $15 if a customer was ill. A sticker on each package said to “Expect a Miracle,” and Pryor repeated this claim in various interviews.
Source: New study explains why having a lower calorie intake is healthier for you – NaturalNews.com
by: RJ Jhonson
Friday, December 14, 2018

A study from the University of Geneva (UNIGE) backs the age-old knowledge that losing weight requires reducing your caloric intake. However, the researchers say it’s not so your body doesn’t get more than it can burn – rather, it’s because eating fewer calories is what’s good for the bacteria in your gut.
The traditional view on weight loss is straightforward – physical activity burns calories you take in through food. If your caloric intake is so high that your body cannot use all of the energy from the food you eat, the surplus calories become stored as fat. Losing weight, therefore, means eating less and moving more so that no surplus is created in the long run.
The researchers from the UNIGE study say this is merely one side of the picture. They restricted the caloric intake of mice for 30 days and found that the animals had developed beige fat. Unlike white fat that stores energy, beige and brown fats burn energy and are beneficial to weight loss.
They then obtained caecum microbial communities from the calorie-restricted mice and transferred these to sterile mice that had no microbes living in their gut yet. They noted that despite eating regularly, the recipient rats also developed beige fats and appeared leaner than normal. They took this as a sign that just changing the composition of the gut microbiome can have a profound effect on the ability of animals to burn fat and lose weight.
The researchers observed many beneficial changes in the mice going through the calorie-restricted diet. Apart from having more beige fat, they also showed signs of lower blood sugar and the ability to burn more fat. They were also more resistant to cold temperatures.
Low calories create compounds for treating obesity
Gram-negative gut bacteria produce lipopolysaccharides (LPS), endotoxins linked to various diseases. Because of their potential risks, LPS automatically trigger an immune response against their source when levels get too high.
Interestingly, the bacteria in calorie-restricted mice produce fewer LPS than in normal mice. When the researchers restored the levels of LPS to normal levels, the mice lost the benefits they gained from their calorie-restricted diet.
What this means, according to the researchers, is that the immune system does more than controlling the body’s reaction to pathogens, it also regulates metabolism. By lowering the levels of LPS produced by gut bacteria, it’s possible to simulate the calorie-restricted state and reap its many health benefits.
The team is now looking into the possibility of using two specific compounds to directly reduce the concentration of LPS and put into action the benefits of a calorie-restricted diet. They offered that there may come a day when this approach is the norm for treating obesity. (Related: Obesity is a social thing: Study finds health habits are “contagious” and highly influenced by social groups.)
Caring for your gut bacteria
Like pets, you need to pay extra attention to the bacteria in your gut and their needs if you want to obtain the benefits they offer. The following are steps to support a healthy gut microbiome.
- Eat healthily – Fruits and vegetables, as well as whole grains, need to be a big part of your diet. These contain dietary fibers that your body cannot digest, but your gut bacteria can use as food. Try to diversify your food choices, too, as this will result in a more diverse microbiome that can protect you from various types of diseases.
- Eat fermented food – Eating fermented food is one of the easiest ways to keep your probiotic populations replenished. Foods like yogurt, sauerkraut, and kimchi are full of probiotics and nutrients that support proper digestion and better overall health.
- Eat foods rich in polyphenols – These are natural compounds that play several roles in the human body. For the most part, they are antioxidants that help protect the body from common diseases. Because they are not digested easily, they also serve as food for gut bacteria.
Learn about the benefits of gut bacteria in terms of weight loss at Slender.news.
Sources include:
Six artificial sweeteners – aspartame, sucralose, saccharine, neotame, advantame, and acesulfame potassium-k – are toxic to gut bacteria

It’s one of the most popular soft drinks in the world, but it seems that Diet Coke may not be as safe as we think.
A new study has revealed that artificial sweeteners found in the drink are toxic to digestive gut microbes.
Researchers from Ben-Gurion University of the Negev found that six artificial sweeteners – aspartame, sucralose, saccharine, neotame, advantame, and acesulfame potassium-k – are toxic to bacteria found in the digestive system.
Continue:
Source link
Mac Slavo
April 17th, 2018

An infectious flesh-eating ulcer caused by a bacteria is spreading so quickly through Australia that scientists in the state of Victoria are declaring this outbreak an epidemic. Normally abundant in West and central Africa and, the buruli ulcer is now taking hold in the “land down under.”
In a study published Monday in the Medical Journal of Australia, the authors caution that the outbreak of the ulcers, described as an “epidemic” in the study, requires an “urgent scientific response.” They report that Victoria is facing a worsening epidemic “defined by cases rapidly increasing in number, becoming more severe in nature, and occurring in new geographic areas.”
Buruli ulcer is caused by infection with the organism Mycobacterium ulcerans. It often affects the skin by deteriorating the tissue, but can go so deep it affects the bone structure. The organism belongs to the family of bacteria that causes tuberculosis and leprosy. However, M. ulcerans is an environmental bacterium and the mode of transmission to humans remains unknown. The organism produces a unique toxin – mycolactone – which causes tissue damage and inhibits the immune response.
According to numbers reported by CNN, in 2016, there were 182 new cases reported, a spike of 72%. But even this number was dwarfed by a further increase of 51% from November 2016 to the same month a year later. In November 2016, there were 156, which rose to 236 cases.
“In Australia, it seems more to be a terrestrial transmission whereas in Africa, for example, the strain is very different and is mostly transmitted through aquatic ecosystems,” said Andres Garchitorena, a researcher at the Institute of Research and Development in France and an expert on Buruli ulcers, who was not involved in the most recent report.
But the cases in Australia are becoming more severe and doctors also do not know the reason. “One possibility is maybe there’s some resistance to the antibiotics that they are using,” Garchitorena said. “It is difficult to prevent a disease when it is not known how infection is acquired,” wrote the lead author and associate professor Daniel O’Brien, an infectious diseases consultant.
Although some deaths from the infection have been reported, most cases are not life-threatening, according to Garchitorena. “There are cases where people have died, but the most common outcome when it’s not treated is a handicap: People may need an amputation or surgery with functional limitations for life,” he said. WHO also reports management of the buruli ulcer becomes more difficult when the patient is dealing with a coinfection of HIV, perhaps lending to the increased severity of the infections in Africa, although that’s largely speculation as still more in-depth studies of this disease are warranted.
The majority of cases are still being reported in West and Central Africa, including Benin, Cameroon, Côte d’Ivoire, the Democratic Republic of the Congo and Ghana. There are no predictable trends in the number of cases reported yearly either.
preventdisease.com
Karen Foster
Dec 20, 2017
At one point or another, we’ve all made a long list of New Year’s resolutions to improve our health and lost weight. Most of these resolutions will fail because support systems are not in place from the start. However a different type of resolution, one for your gut bugs is far more effective than any strategy for weight loss.

There are over 400 species of bacteria in your belly right now that can be the key to health or disease.
The genomes of the bacteria and viruses of the human gut alone are thought to encode 3.3 million genes.
At this very moment, there are trillions of bacteria living in your body — the majority in your gastrointestinal (GI) tract. Collectively, these bacteria are known as the microbiome. The bulk of them are symbiotic — in other words, mutually beneficial. We help our microbiome survive and it helps us survive. Researchers are continually uncovering diverse and important functions of the microbiome related to energy metabolism, immunity, GI and mental health — among others.
Weight loss resolutions are relevant in this regard, since the gut microbiome affects the rate of absorption, metabolism and storage of calories. For example, specific bacterial strains, such as Firmicutes and Bacteroidetes, shift during obesity — potentially increasing energy harvest from food. Ai-Ling Lin, assistant professor at the UK Sanders Brown Center on Aging, is investigating the impact of the microbiome on the aging brain and mental health. Her research findings demonstrate a healthy microbiome is associated with reduced anxiety and risk for dementia with aging. A well-known role of the gut microbiome is protection of the GI tract’s health and function. This is why some antibiotics can cause loose stools or diarrhea. Of note, probiotic supplementation has been shown to be effective in the treatment of antibiotic-associated diarrhea.
Maximize your beneficial and defensive features of the microbiome by nourishing and protecting it, every single day. Here are some tips to nurture the good bugs within during the coming year:
Choose Complex Carbohydrates
A primary source of energy for the microbiome is complex carbohydrates. Vegetables, fruits, legumes, seeds and nuts are sources of resistant starch and dietary fiber — also known as “prebiotics.” Prebiotic-rich foods (not refined, sugary foods) give gut bugs plenty of fuel to flourish.
Include Natural Probiotics In Your Diet
Enrich the microbiome with a serving of yogurt, kefir, sauerkraut or fermented vegetables regularly. Beyond vitamins and minerals, these foods are rich sources of beneficial bacteria such as Lactobacillus and Bifidobacterium, which may boost immunity and overall health. Effects of probiotics vary from person to person, since everyone’s microbiome is unique.
Get Plenty of Sleep
Even gut bugs need a good night’s rest. The microbiome shifts in composition and function during the light versus dark-hours of the day. Research indicates that irregular circadian rhythms (associated with jet lag in frequent flyers, for example) leads to shifts in the microbiome associated with metabolic changes. Taking steps toward a good night’s sleep will safeguard your gut bugs’ health and functionality.
Probiotic Sources
Cultured dairy products like yogurt, acidophilus milk, buttermilk, sour cream, cottage cheese and kefir are the best known food sources of friendly bacteria. Equally effective probiotic food sources include cultured/fermented vegetables (cabbage, turnips, eggplant, cucumbers, onions, squash, and carrots). Other, lesser known or used food sources of probiotics are sauerkraut and sourdough breads. Ideally, one could get a good supply of probiotics from one or more of these diverse foodstuffs. If dietary sources are not easily available, supplemental probiotic powders and capsules are good alternatives. Choose a brand that has at least 3 different strains of friendly bacteria and between 6 — 15 billion live organisms.
A diet high in beneficial fats may help stem the growth of harmful gut bacteria that trigger the onset of Crohn’s disease.
NaturalNews.com
by: Russel Davis
December 08, 2017

(Natural News) A diet high in beneficial fats may help stem the growth of harmful gut bacteria that trigger the onset of Crohn’s disease, according to a study carried out by a team of researchers at the Case Western Reserve University School of Medicine in Cleveland, Ohio. Crohn’s disease is a type of inflammatory bowel syndrome that is characterized by intestinal cramps, diarrhea, and debilitating inflammation of the intestinal tract. The disease currently affects up to half a million people across the U.S. However, the scientific community maintains that the cause of the disease remains unclear, the experts report.
The research team examined the effects of plant-derived beneficial fats — such as coconut oil or cocoa butter — on animal models as part of the study. The scientists observed that the good fats significantly reduced the bacterial diversity in mice with Crohn’s-like disease. According to the researchers, mice models that are subjected to beneficial fatty diets exhibited up to 30 percent fewer kinds of gut bacteria compared with those that followed a normal diet. This in turn led to a relatively different gut microbiome composition in the animal models, the experts added.
The scientists observed that the marked changes in gut bacterial composition could be seen in the animals’ feces. Likewise, other altered bacterial species were observed in the cecum, a portion of the intestine that usually becomes swollen in Crohn’s disease patients. The research team also observed that even modest levels of beneficial fats may still promote gut health. According to the researchers, mice given low concentrations of coconut oil or cocoa butter exhibited less severe inflammation in the small intestine.
“The finding is remarkable because it means that a Crohn’s patient could also have a beneficial effect on their gut bacteria and inflammation by only switching the type of fat in their diet. Patients would only need to replace a ‘bad’ fat with a ‘good’ fat, and eat normal amounts,” says Alexander Rodriguez-Palacios, study author and an assistant professor of medicine at the university.
The findings may help health care providers identify target bacteria to use in probiotics treatment to alleviate inflammatory bowel syndromes in affected patients, Rodriguez-Palacios says.
“Ongoing studies are now helping us to understand which component of the ‘good’ and ‘bad’ fats make the difference in the gut microbes and make mice healthier. Ultimately, we aim to identify the ‘good’ fat-loving microbes for testing as probiotics,” Rodriguez-Palacios adds.
However, the expert has also cautioned that the findings may have varying effects on Crohn’s disease patients.
“Not all ‘good’ fats might be good in all patients. Mice indicate that each person could respond differently. But diet is something we are very hopeful could help at least some patients without the side-effects and risks carried by drugs. The trick now is to really discover what makes a fat ‘good’ or ‘bad’ for Crohn’s disease,” the expert explains.
The findings were presented at the annual Digestive Disease Week conference in Chicago in June 2017. The study serves as a pioneering research on the correlation between gut microbiome changes and overall intestinal health in Crohn’s disease patients. The study is also the first to demonstrate how high-fat diets can change gut bacteria composition in order to keep inflammation at bay. In addition, the research is one of the six studies accepted for scientific conference presentation that have been produced by the university.
Sources include:
“Whenever bacteria such as Salmonella invade the body, around a third of the bugs ‘cloak’ themselves as a defence mechanism against the body’s immune system. They enter a type of stand-by mode possibly to hide from the body’s immune system, that means they are not killed by antibiotics. The bacteria stop replicating and can remain in this dormant state for days, weeks or even months. When the immune system attack has passed, some bacterial cells spring back to life and trigger another infection.”
With permission from
by: Zoey Sky
December 04, 2017
(Natural News) According to a study published in 2016, scientists have discovered a bacteria “alarm clock” that can wake dormant Salmonella in the body which enables the bug to trigger a relapse.
The researchers from Imperial College London say that the “alarm clock” is common among various types of bacteria, such as Salmonella and E. coli. Their discovery could explain why some people suffer repeated bouts of infections, like ear or urinary tract infections, even though they take antibiotics. The team aims to use these findings to look into “hard-to-treat infections.”
Dr. Sophie Helaine, the lead author of the research from the Department of Medicine at Imperial, said, “Whenever bacteria such as Salmonella invade the body, around a third of the bugs ‘cloak’ themselves as a defence mechanism against the body’s immune system. They enter a type of stand-by mode possibly to hide from the body’s immune system, that means they are not killed by antibiotics. The bacteria stop replicating and can remain in this dormant state for days, weeks or even months. When the immune system attack has passed, some bacterial cells spring back to life and trigger another infection.”
Dr. Helaine continued, “This is why, for instance, a woman may think she has recovered from a urinary tract infection – and yet days or weeks later it seems to return. Many patients may assume it’s a different infection – but actually it’s the same bug.” (Related: Boosting immune system with natural methods offers many health benefits.)
She adds that these so-called persistent bacteria also “fuel antibiotic resistance,” and this is why patients end up taking many courses of antibiotics for one infection. Taking this amount of antibiotics means that some bacteria are “developing resistance.”
Earlier research from Dr. Helaine’s lab determined that Salmonella bacteria go into stand-by mode by “poisoning” themselves using toxins.
In the current study, the team showed a mechanism that Salmonella use “to detoxify themselves.” This wakes them from stand-by and lets them start growing again.
Dr. Helaine said it is possible that many bacteria use this same toxin, called TacT, to “switch into stand-by mode.” These bacteria include those that cause many intestinal, ear, throat, or urinary tract infections and even tuberculosis.
Dr. Helaine shares that if they can determine how to control this particular mechanism and “force the bacteria out of stand-by” they can then be treated with antibiotics, effectively killing them.
For the study, Dr. Helaine et al. used Salmonella cells in the laboratory to identify the bacterial alarm clock. The team tested a collection of over 4,000 proteins to look for those that wake the bacteria up. They isolated an enzyme called peptidyl-tRNA hydrolase (Pth) that was an effective alarm clock.
The scientists have determined that the toxin TacT “stops cell growth during times of attack by blocking protein production.” When the conditions are more suitable for cell growth, Pth molecules eliminate the block on protein production and lets the growth continue.
Dr. Helaine concluded, “When the bacteria are under attack they go to sleep and wait for better days. Then once the immune system attack has passed, the body is once again a favourable place to start an infection, and cell growth resumes.”
Boost your immune system naturally
Don’t wait until you need antibiotics to get better. Try these natural tips to boost your immune system instead:
- Get a good night’s rest and manage stress — Sleep deprivation and stress overload increase the hormone cortisol, prolonged elevation of which can suppress immune function.
- Quit smoking or avoid second-hand tobacco smoke — Smoking undermines basic immune defenses and increase raises the risk of bronchitis and pneumonia in everyone and middle ear infections in children.
- Eat healthier — Add plenty of vegetables, fruits, nuts, and seeds to your diet so your body has all the nutrients your immune system needs.
You can read more articles about preventing infections and illness at Prevention.news.
Sources include:
Published on 7 Aug 2017
Source: Mystery of animals’ appearance on Earth solved by ‘pivotal’ study — RT Viral
RT Viral

A research team from the Australian National University (ANU) studied ancient molecules buried in the rocks and discovered that a very particular set of circumstances led to the origin of life on our planet.
It all started about 700 million years ago when the world was covered in ice, a period called “Snowball Earth.”
“The Earth was frozen over for 50 million years,” explains ANU Associate Professor Jochen Brocks.
“Huge glaciers ground entire mountain ranges to powder that released nutrients, and when the snow melted during an extreme global heating event rivers washed torrents of nutrients into the ocean.”
This abundance of nutrients triggered the key moment for the development of life on Earth – the rise of algae.
Dr Brocks said this extraordinary algae bloom kicked off a “revolution of ecosystems” which was “one of the most profound ecological revolutions in Earth’s history.”
The extremely high levels of nutrients in the ocean, and cooling of global temperatures, created the perfect conditions for the rapid spread of algae.
This led to a dramatic shift where the oceans went from being dominated by bacteria to a world inhabited by more complex life.
The phenomenon was so critical that humans and other animals would simply not exist had it not taken place, the researchers point out.
“These large and nutritious organisms at the base of the food web provided the burst of energy required for the evolution of complex ecosystems, where increasingly large and complex animals, including humans, could thrive on Earth,” Dr Brocks said.
The research is published in Nature, and the team’s findings will be presented at a conference in Paris next week.
Yes they do, just look at the Royal parasites from England…Hehehe
Source: Do Parasites Rule The World By Using Our Bodies As Hosts? – Collective Evolution
http://www.collective-evolution.com

“The parasite grows in a rodent, but it needs to get into a cat somehow to reproduce,” says Shelley Adamo, a biologist who studies neuroparasitology at Dalhousie University in Halifax, Canada. “When a rat becomes infected, the parasite somehow makes rats become attracted to cat urine, when it would normally avoid it.”
Estimates from the Centre for Disease Control (CDC) suggest that more than 60 million Americans carry the single-celled parasite, most often obtained through ingesting undercooked meat or interacting with cats. The CDC claims that “of those who are infected very few have symptoms because a healthy person’s immune system usually keeps the parasite from causing illness.” This new information may force scientists to reconsider that statement, however.
New Research on Parasites
A study published in the Journal of Experimental Biology by Jaroslav Flegr, a scientist at Charles University in Prague, suggests that people who are infected with this parasite have slower reaction times and are often “less altruistic” than uninfected people.
Researchers determined that women who were infected with Toxoplasma “more often report that diplomacy is not their strong point” and that “some people have the power to impose their will on others with hypnosis.” They also described women having “a weak instinct for self-preservation: in situations where somebody else might be afraid, for example being alone in a forest or in an empty house at night, they remain calm.”
Flegr acknowledges that they “cannot distinguish whether the observed changes are manifestations of the manipulative activity or only symptoms of the chronic disease” often caused by Toxoplasma, but Toxoplasma infection’s prevalence, nevertheless, makes it an ideal “model for studying manipulative activity in humans.” There are a “large number of parasitic organisms … that may influence the human host even more than the Taxoplasma,” he continues.
Continue:
Do Parasites Rule The World By Using Our Bodies As Hosts? – Collective Evolution
It helped them conquer the world, three billion years ago.
Source: Microbes have their own version of the internet
theconversation.com
Senior Lecturer in Biology, Brunel University London
Aug 7, 2017
Creating a huge global network connecting billions of individuals might be one of humanity’s greatest achievements to date, but microbes beat us to it by more than three billion years. These tiny single-celled organisms aren’t just responsible for all life on Earth. They also have their own versions of the World Wide Web and the Internet of Things. Here’s how they work.
Much like our own cells, microbes treat pieces of DNA as coded messages. These messages contain information for assembling proteins into molecular machines that can solve specific problems, such as repairing the cell. But microbes don’t just get these messages from their own DNA. They also swallow pieces of DNA from their dead relatives or exchange them with living mates.
These DNA pieces are then incorporated into their genomes, which are like computers overseeing the work of the entire protein machinery. In this way, the tiny microbe is a flexible learning machine that intelligently searches for resources in its environment. If one protein machine doesn’t work, the microbe tries another one. Trial and error solve all the problems.
But microbes are too small to act on their own. Instead, they form societies. Microbes have been living as giant colonies, containing trillions of members, from the dawn of life. These colonies have even left behind mineral structures known as stromatolites. These are microbial metropolises, frozen in time like Pompeii, that provide evidence of life from billions of years ago.

Microbial colonies are constantly learning and adapting. They emerged in the oceans and gradually conquered the land – and at the heart of their exploration strategy was information exchange. As we’ve seen, individual members communicate by exchanging chemical messages in a highly coordinated fashion. In this way, microbial society effectively constructs a collective “mind”.
This collective mind directs pieces of software, written in DNA code, back and forth between trillions of microbes with a single aim: to fully explore the local environment for resources using protein machines.
When resources are exhausted in one place, microbial expedition forces advance to find new lands of plenty. They transmit their discoveries back to base using different kinds of chemical signals, calling for microbial society to transform from settlers to colonisers.
In this way, microbes eventually conquered the entire planet, creating a global microbial network that resembles our own World Wide Web but using biocehmical signals instead of electronic digital ones. In theory, a signal emitted in waters around the South Pole could effectively travel fast to waters around the North Pole.
Internet of living things
The similarities with human technology don’t stop there. Scientists and engineers are now working on expanding our own information network into the Internet of Things, integrating all manner of devices by equipping them with microchips to sense and communicate. Your fridge will be able to alert you when it is out of milk. Your house will be able to tell you when it is being burgled.
Microbes built their version of the Internet of Things a long time ago. We can call it the “Internet of Living Things”, although it’s more often known as the biosphere. Every organism on the planet is linked in this complex network that depends on microbes for its survival.
More than a billion years ago, one microbe found its way inside another microbe that became its host. These two microbes became a symbiotic hybrid known as the eukaryotic cell, the basis for most of the lifeforms we are commonly familiar with today. All plants and animals are descended from this microbial merger and so they contain the biological “plug-in” software that connects them to the Internet of Living Things.

For example, humans are designed in a way that means we cannot function without the trillions of microbes inside our bodies (our microbiome) that help us do things like digest food and develop immunity to germs. We are so overwhelmed by microbes that we imprint personal microbial signatures on every surface we touch.
The Internet of Living Things is a neat and beautifully functioning system. Plants and animals live on the ecological waste created by microbes. While to microbes, all plants and animals are, as author Howard Bloom puts it, “mere cattle on whose flesh they dine”, whose bodies will be digested and recycled one day.
Microbes are even potential cosmic tourists. If humans travel into deep space, our microbes will travel with us. The Internet of Living Things may have a long cosmic reach.
The paradox is that we still perceive microbes as inferior organisms. The reality is that microbes are the invisible and intelligent rulers of the biosphere. Their global biomass exceeds our own. They are the original inventors of the information-based society. Our internet is merely a by-product of the microbial information game initiated three billion years ago.
“Journalists…suspect that the local population is suffering from the spread of Cynthia, the runaway flesh eating bacteria that was bred on demand by BP (British Petroleum) to combat its major oil spill in the same area back in 2010.”
“The fact that Cynthia was created in secret US laboratories only to be unleashed in the region without any prior studies into the possible consequences has already been reported.”
Source: Cynthia, the Runaway Fleshing Eating Bacteria, is Claiming American Lives | New Eastern Outlook
The Alabama Department of Public Health has recently announced that has observed a new pandemic involving a potentially deadly flesh eating virus spreading like wild fire in the Gulf of Mexico area. The majority of those infected were swimming in the Gulf of Mexico, and had minor cuts or bruisers or ate raw seafood from this area. Upon infecting a human being the so-called vibrio compromises kidney and liver functions before spreading further.
It’s been reported that symptoms include nausea, vomiting, fever, chills, blisters around the wounded areas infected, swelling and redness. American health officials claim that 80% of the time, if people receive medical assistance within the first 24 hours of infection, they should be fine. They suggest treating the affected area immediately after contamination, including thoroughly washing the area with soap and water and disinfecting it with rubbing alcohol. However, this infection is highly resistant to antibiotics and if a person infected fails to seek medical assistance within the above mentioned time window, chances of surviving the so-called vibrio in most cases barely reaches 50%.
However, it’s rarely reported that if a person was infected via cuts or bruisers on their limb, the infected areas are transformed into un-treatable swelling ulcers that force medical practitioners to amputate the infected limb in a bid to save the patient’s life. Colonies of this bacteria grow rapidly in warm water, so the majority of infection cases occur in summer. Those who are living along the Gulf of Mexico coastline are increasingly concerned for their well being, no longer eating raw seafood and avoiding the seashore altogether. Local health authorities have reported dozens of cases this year alone.
However, there’s a number of journalists that remain convinced that those who were infected by a flesh eating bacteria are not suffering from the relatively harmless Vibrio Vulnificus, instead they suspect that the local population is suffering from the spread of Cynthia, the runaway flesh eating bacteria that was bred on demand by BP (British Petroleum) to combat its major oil spill in the same area back in 2010.
The fact that Cynthia was created in secret US laboratories only to be unleashed in the region without any prior studies into the possible consequences has already been reported. It’s clear now that oil spills were only the beginning, since now this bacteria is eating sea creatures and humans alike. The artificially created monster leaves little chance for survival to fish or seals, leaving both covered in swelling ulcers within hours after entering an infected area.
“Cynthia” is a synthetic bacteria, an artificial organism with an artificially engineered genome. Such artificial cells are rapidly multiplying, due to the properties of self-reproduction that were provided during the early stages of their design.
It’s curious that the entire coastline of the Gulf of Mexico is now covered with brownish, oily balls. According to a local chemist Bob Naman, those would infect anyone unfortunate enough to break them with their unprotected hands or would otherwise contact them. Should a person have an open wound, the contents of the ball will go straight into one’s system, warns the scientist.
A local blogger and activist, Alexander Higgins has cited a study conducted by to Columbia University, according to which after the oil spill in 2010, 40% of residents residing near the Gulf of Mexico acquired respiratory and skin diseases, and one in four thinks of leaving their current place of residence.
Cases of massive bird deaths, like the ones in Arkansas and New Orleans, just like massive fish deaths in the same region, are usually associated by the American media with Cynthia. However, when people become covered in ulcers only to die in agony after swimming in the Gulf of Mexico, they are being described as the victims of an unknown decease. Those infected have little chance of survival since Cynthia compromises their internal organs, causing profuse internal bleeding and death. Yet, the true scale of the tragedy remains hidden, while any mentions of human deaths caused by Cynthia are being suppressed at a governmental level.
Jean Périer is an independent researcher and analyst and a renowned expert on the Near and Middle East, exclusively for the online magazine “New Eastern Outlook“.
Source: Peer Into the Post-Apocalyptic Future of Antimicrobial Resistance | WIRED
wired.com
Michael T. Osterholm & Mark Olshaker
March 18, 2017
About 4 million years ago, a cave was forming in the Delaware Basin of what is now Carlsbad Caverns National Park in New Mexico. From that time on, Lechuguilla Cave remained untouched by humans or animals until its discovery in 1986—an isolated, pristine primeval ecosystem.
When the bacteria found on the walls of Lechuguilla were analyzed, many of the microbes were determined not only to have resistance to natural antibiotics like penicillin, but also to synthetic antibiotics that did not exist on earth until the second half of the twentieth century. As infectious disease specialist Brad Spellberg put it in the New England Journal of Medicine, “These results underscore a critical reality: antibiotic resistance already exists, widely disseminated in nature, to drugs we have not yet invented.”
The origin story of antibiotics is well known, almost mythic, and antibiotics, along with the other basic public health measures, have had a dramatic impact on the quality and longevity of our modern life. When ordinary people called penicillin and sulfa drugs miraculous, they were not exaggerating. These discoveries ushered in the age of antibiotics, and medical science assumed a lifesaving capability previously unknown.

Note that we use the word discoveries rather than inventions. Antibiotics were around many millions of years before we were. Since the beginning of time, microbes have been competing with other microbes for nutrients and a place to call home. Under this evolutionary stress, beneficial mutations occurred in the “lucky” and successful ones that resulted in the production of chemicals—antibiotics—to inhibit other species of microbes from thriving and reproducing, while not compromising their own survival. Antibiotics are, in fact, a natural resource—or perhaps more accurately, a natural phenomenon—that can be cherished or squandered like any other gift of nature, such as clean and adequate supplies of water and clean air.
Equally natural, as Lechuguilla Cave reminds us, is the phenomenon of antibiotic resistance. Microbes move in the direction of resistance in order to survive. And that movement, increasingly, threatens our survival.
With each passing year, we lose a percentage of our antibiotic firepower. In a very real sense, we confront the possibility of revisiting the Dark Age where many infections we now consider routine could cause severe illness, when pneumonia or a stomach bug could be a death sentence, when a leading cause of mortality in the United States was tuberculosis.
The Review on Antimicrobial Resistance (AMR) determined that, left unchecked, in the next 35 years antimicrobial resistance could kill 300,000,000 people worldwide and stunt global economic output by $100 trillion. There are no other diseases we currently know of except pandemic influenza that could make that claim. In fact, if the current trend is not altered, antimicrobial resistance could become the world’s single greatest killer, surpassing heart disease or cancer.
In some parts of the United States, about 40 percent of the strains of Streptococcus pneumonia, which the legendary nineteenth and early twentieth century physician Sir William Osler called “the captain of the men of death,” are now resistant to penicillin. And the economic incentives for pharmaceutical companies to develop new antibiotics are not much brighter than those for developing new vaccines. Like vaccines, they are used only occasionally, not every day; they have to compete with older, extremely cheap generic versions manufactured overseas; and to remain effective, their use has to be restricted rather than promoted.
As it is, according to the CDC, each year in the United States at least 2,000,000 people become infected with antibiotic-resistant bacteria and at least 23,000 people die as a direct result of these infections. More people die each year in this country from MRSA (methicillin-resistant Staphylococcus aureus, often picked up in hospitals) than from AIDS.
If we can’t—or don’t—stop the march of resistance and come out into the sunlight, what will a post-antibiotic era look like? What will it actually mean to return to the darkness of the cave?
Without effective and nontoxic antibiotics to control infection, any surgery becomes inherently dangerous, so all but the most critical, lifesaving procedures therefore would be complex risk-benefit decisions. You’d have a hard time doing open-heart surgery, organ transplants, or joint replacements, and there would be no more in vitro fertilization. Caesarian delivery would be far more risky. Cancer chemotherapy would take a giant step backwards, as would neonatal and regular intensive care. For that matter, no one would go into a hospital unless they absolutely had to because of all the germs on floors and other surfaces and floating around in the air. Rheumatic fever would have lifelong consequences. TB sanitaria could be back in business. You could just about do a post-apocalyptic sci-fi movie on the subject.
To understand why antibiotic resistance is rapidly increasing and what we need to do to avert this bleak future and reduce its impact, we have to understand the Big Picture of how it happens, where it happens, and how it’s driven by use in humans and animals.
Human Use
Think of an American couple, both of who work fulltime. One day, their 4-year-old son wakes up crying with an earache. Either mom or dad takes the child to the pediatrician, who has probably seen a raft of these earaches lately and is pretty sure it’s a viral infection. There is no effective antiviral drug available to treat the ear infection. Using an antibiotic in this situation only exposes other bacteria that the child may be carrying to the drug and increases the likelihood that an antibiotic resistant strain of bacteria will win the evolutionary lottery. But the parent knows that unless the child has been given a prescription for something, the daycare center isn’t going to take him and neither partner can take off from work. It doesn’t seem like a big deal to write an antibiotic prescription to solve this couple’s dilemma, even if the odds the antibiotic is really called for are minute.
While the majority of people understand that antibiotics are overprescribed and therefore subject to mounting resistance, they think the resistance applies to them, rather than the microbes. They believe that if they take too many antibiotics – whatever that unknown number might be—they will become resistant to the agents, so if they are promoting a risk factor, it is only for themselves rather than for the entire community.
Doctors, of course, understand the real risk. Are they culpable to the charge of over- and inappropriately prescribing antibiotics? In too many cases, the answer is Yes.
Continue :
Peer Into the Post-Apocalyptic Future of Antimicrobial Resistance | WIRED
A new study reports Parkinson’s disease and some of the medications used to treat the condition have distinct effects on the bacteria that make up the gut microbiome.
Source: Further Evidence For Link Between Gut Bacteria and Parkinson’s Disease – Neuroscience News
neurosciencenews.com
March 3, 2017
Summary: A new study reports Parkinson’s disease and some of the medications used to treat the condition have distinct effects on the bacteria that make up the gut microbiome.
Source: University of Alabama at Birmingham.
There is growing evidence showing a connection between Parkinson’s disease — a neurodegenerative condition — and the composition of the microbiome of the gut. A new study from researchers at the University of Alabama at Birmingham shows that Parkinson’s disease, and medications to treat Parkinson’s, have distinct effects on the composition of the trillions of bacteria that make up the gut microbiome.
The findings were published in February in Movement Disorders, the journal of the International Parkinson and Movement Disorder Society.
“Our study showed major disruption of the normal microbiome ¬ — the organisms in the gut — in individuals with Parkinson’s,” said Haydeh Payami, Ph.D., professor in the Department of Neurology, in the UAB School of Medicine.
Payami says, at this point, researchers do not know which comes first. Does having Parkinson’s cause changes in an individual’s gut microbiome, or are changes in the microbiome a predictor or early warning sign of Parkinson’s? What is known is that the first signs of Parkinson’s often arise as gastrointestinal symptoms such as inflammation or constipation.
“The human gut hosts tens of trillions of microorganisms, including more than 1,000 species of bacteria,” she said. “The collective genomes of the microorganisms in the gut is more than 100 times larger than the number of genes in the human genome. We know that a well-balanced gut microbiota is critical for maintaining general health, and alterations in the composition of gut microbiota have been linked to a range of disorders.”
Payami’s team studied 197 patients with Parkinson’s and 130 controls. Subjects came from Seattle, New York and Atlanta.
The study indicated that Parkinson’s is accompanied by imbalance in the gut microbiome. Some species of bacteria were present in larger numbers than in healthy individuals; other species were diminished. Different medications used to treat Parkinson’s also appear to affect the composition of the microbiome in different ways.
“It could be that, in some people, a drug alters the microbiome so that it causes additional health problems in the form of side effects,” Payami said. “Another consideration is that the natural variability in the microbiome could be a reason some people benefit from a given drug and others are unresponsive. The growing field of pharmacogenomics — tailoring drugs based on an individual’s genetic makeup — may need to take the microbiome into consideration.”
The study subjects came from three regions, the Northeast, Northwest and South. Payami says the research team detected an unexpected difference in gut imbalance as a function of geographic site, which may reflect the environmental, lifestyle and diet differences between the three regions.
Another function of the microbiome is to help the body rid itself of xenobiotics — chemicals not naturally found in the body often arising from environmental pollutants. The study found evidence that the composition of bacteria responsible for removing those chemicals was different in individuals with Parkinson’s. This may be relevant because exposure to pesticides and herbicides in agricultural settings is known to increase the risk of developing Parkinson’s.
Payami says the study of the microbiome is a relatively new field, and a better understanding of macrobiotics may provide unexpected answers for Parkinson’s disease and potentially other disorders.
A better understanding of macrobiotics may provide unexpected answers for Parkinson’s disease and potentially other disorders. NeuroscienceNews.com image is adapted from the UAB press release.
“This opens up new horizons, a totally new frontier,” she said. “There are implications here for both research and treatment of Parkinson’s disease. Therapies that regulate the imbalance in the microbiome may prove to be helpful in treating or preventing the disease before it affects neurologic function.” However, Payami cautions against grand conclusions until more data are available.
Payami says another study is underway at UAB with individuals with Parkinson’s and healthy individuals in Alabama in an effort to replicate and confirm the results.
“The present findings lend support to the notion that the composition of the gut microbiome may hold new information for assessing efficacy and toxicity of Parkinson’s medications,” Payami said. “Additional studies are needed to assess the effects of those drugs, with larger numbers of treated and untreated patients as well as individuals who do not have Parkinson’s.”
Funding: Funding support for the study was provided by National Institutes of Health.
Source: Brian Mullen – University of Alabama at Birmingham
Image Source: NeuroscienceNews.com image is adapted from the UAB press release.
Original Research: Abstract for “Parkinson’s disease and Parkinson’s disease medications have distinct signatures of the gut microbiome” by Erin M. Hill-Burns PhD, Justine W. Debelius PhD, James T. Morton BS, William T. Wissemann BA, Matthew R. Lewis MS, Zachary D. Wallen MS, Shyamal D. Peddada PhD, Stewart A. Factor DO, Eric Molho MD, Cyrus P. Zabetian MD, MS, Rob Knight PhD, and Haydeh Payami PhD in Movement Disorders. Published online February 14 2017 doi:10.1002/mds.26942
Source: China on the verge of a widespread superbug pandemic thanks to spreading MCR-1 gene
newstarget.com

A gene that confers resistance to colistin, the “antibiotic of last resort,” is alarmingly widespread in China, according to two separate studies published in The Lancet on January 27.
The drug-resistance gene in question, MCR-1 was first identified in China in 2015, in Escherichia coli (more commonly known as E. coli) bacteria in pigs, pork, and a handful of human patients. Since then, the gene has turned up in 30 other countries, including the United States. It renders bacteria immune to one of the few antibiotics that can still be used against multidrug resistant superbugs.
“This is a warning shot about the possible scenario where we don’t have very much left in the armory to treat infections,” said Nigel Brown of Britain’s Microbiology Society.
Gene already spreading to superbugs
In the first study, researchers collected more than 17,000 samples from patients with gut bacteria infections at two hospitals in Zhejiang and Guangdong from 2007 to 2015. Overall, they found that about 1 percent of the infectious bacteria sampled contained the MCR-1 gene. The gene was more common in E. coli, with a frequency of 1.4 percent. Notably, the prevalence of MCR-1 in E. coli increased over the study period.
The researchers found that people with a recent history of antibiotic use were significantly more likely to be infected with MCR-1 positive E. coli. There was no increased risk associated with living near a farm, even though colistin has been widely used in Chinese agriculture. This suggests that MCR-1 is likely spreading between bacteria, rather than MCR-1 positive bacteria merely spreading through asexual reproduction.
This mode of transmission is particularly worrisome because it is faster and also makes it more likely that MCR-1 will cross to other strains and species of bacteria, including those already resistant to other antibiotics. This could easily produce a superbug resistant to all known human antibiotics.
This has already started occurring in China, the second study found. In that study, researchers screened more than 2,000 bacterial samples from bloodstream infection patients at 28 Chinese hospitals from 2013 to 2014. They found that about 1.3 percent of E. coli samples were positive for MCR-1; a similar rate to the first study. This indicated that MCR-1 has already spread across China, and may be spreading through contaminated medical equipment.
Significantly, many of the positive samples were of a strain known as ST131, which is already multidrug resistant. E. coli ST131 is a major cause of urinary tract infections worldwide.
“Nightmare bacteria” in our future
Many researchers have blamed the rapid spread of MCR-1 on China’s widespread use of colistin as a growth-promoter for livestock. China finally banned the drug from animal feed in 2016, but it may be too late to stop the gene’s spread. And while MCR-1 remains relatively rare in bacteria that infect humans, the bacterial ability to swap DNA between unrelated species likely makes it only a matter of time before the gene crosses to more common human infectious agents.
“It now looks like there’s potential for the resistance gene to move around and spread between different species of bacteria,” Brown said.
And now that colistin has been approved in China for human use, the spread of colistin-resistance is expected to accelerate.
A preview of what this might look like came in August, when the CDC analyzed samples of the Klebsiella pneumoniae bacteria that had killed a 70-year-old Reno woman from blood poisoning. They found that the bacteria were resistant to all 26 antibiotics approved for use in human beings, including “colistin.” The CDC dubbed the strain a “nightmare bacteria.”
Experts are warning with increasing urgency that unless dramatic changes are made to antibiotic prescribing practices, including curtailing the use of drugs in agriculture, we may soon enter a post-antibiotic era. This would render currently routine medical procedures such as surgery and cancer treatment so unsafe as to be impossible.
Sources for this article include:


















